1. Introduction: De-Mystifying the Root Canal
Of all the procedures in modern dentistry, perhaps none is more misunderstood or unjustly feared than the root canal. For generations, jokes and media portrayals have associated root canals with extreme pain. In reality, the exact opposite is true.
It is the infection inside your tooth that causes the agonizing, sleep-depriving pain that sends you rushing to the dentist. A Root Canal Treatment (Endodontic Therapy) is the highly advanced, modern solution designed to instantly eliminate that pain and preserve your natural tooth, saving it from the surgeon’s pliers.
At Anatolia Smile, our specialized endodontic team utilizes state-of-the-art diagnostic imaging, profound anesthesia protocols, and microscopic rotary instruments to perform root canals that are swift, highly predictable, and—most importantly—completely painless. We believe that no artificial implant can perfectly replicate the biomechanics of your natural tooth, and we fight to save your biological smile whenever possible.
2. Anatomy of an Infection: Why Do You Need a Root Canal?
To understand how a root canal works, you must understand the anatomy of a tooth.
A tooth is not a solid piece of bone. The white part you see is the Enamel (the hardest substance in the human body). Beneath the enamel is a softer layer called Dentin. In the very center of the tooth, running all the way down through the roots into the jawbone, is a hollow chamber called the Pulp Canal.
This pulp contains blood vessels, connective tissue, and highly sensitive nerve fibers. These nerves are vital while the tooth is growing in childhood, but once the tooth is fully mature, it can successfully survive without the internal pulp, relying instead on the nourishment from the surrounding gum and bone tissue.
A root canal becomes absolutely necessary when this internal pulp becomes damaged, inflamed, or infected. This occurs through three primary pathways:
- Deep Decay (Cavities): If a cavity is left untreated, the bacteria will eat through the enamel and dentin until they breach the center pulp chamber. Once bacteria invade the pulp, the soft tissues become aggressively infected and die.
- Repeated Dental Trauma: Every time a tooth is drilled (such as replacing old, massive amalgam fillings), it traumatizes the nerve. Over time, the nerve can succumb to this cumulative stress and die silently.
- Physical Cracks or Fractures: If you bite down on an olive pit and crack the tooth, the microscopic crack acts as a highway for mouth bacteria to travel directly into the pulp chamber, leading to rapid infection.
The Symptoms: When the pulp becomes infected, gas and pus build up inside the rigid tooth structure. Because the tooth cannot expand, this creates immense internal pressure on the dying nerve. This causes excruciating, throbbing pain, extreme lingering sensitivity to hot and cold, swelling in the gums (an abscess), and pain when tapping or chewing on the tooth.
3. The Endodontic Solution: Saving the Shell
If the dying pulp is left inside the tooth, the infection will eventually travel down the root canals and exit the tip of the root, forming a painful abscess (a pocket of pus) in the jawbone. If ignored, the infection can erode the jawbone and even spread to the bloodstream, causing serious systemic health issues.
Historically, the only way to cure this infection was to pull the entire tooth. Endodontic therapy offers a brilliant alternative: we remove the infected tissue from the inside of the tooth while leaving the hard, healthy outer shell undisturbed in your jaw.
4. The Anatolia Smile Root Canal Protocol
Our endodontic specialists utilize a highly precise, technology-driven workflow:
Phase 1: 3D Diagnostics & Absolute Anesthesia Before we begin, we take high-resolution digital X-rays (and often a 3D CBCT scan for complex molars). This allows the endodontist to map the exact number of roots, their length, and any microscopic curves or hidden canals.
We then apply a potent topical numbing gel, followed by the careful administration of computer-assisted local anesthesia. We will profoundly numb the tooth, the surrounding bone, and all associated nerve pathways. We will test the tooth to guarantee you feel zero sensation before proceeding.
Phase 2: Isolation (The Dental Dam) This is a critical step that many older clinics skip. We place a “dental dam”—a small, stretchy sheet of rubber—around the infected tooth. This serves two vital purposes: it prevents you from swallowing any tiny instruments or bad-tasting antibacterial fluids, and it keeps your saliva (which is full of bacteria) from entering the completely sterile surgical field inside the tooth.
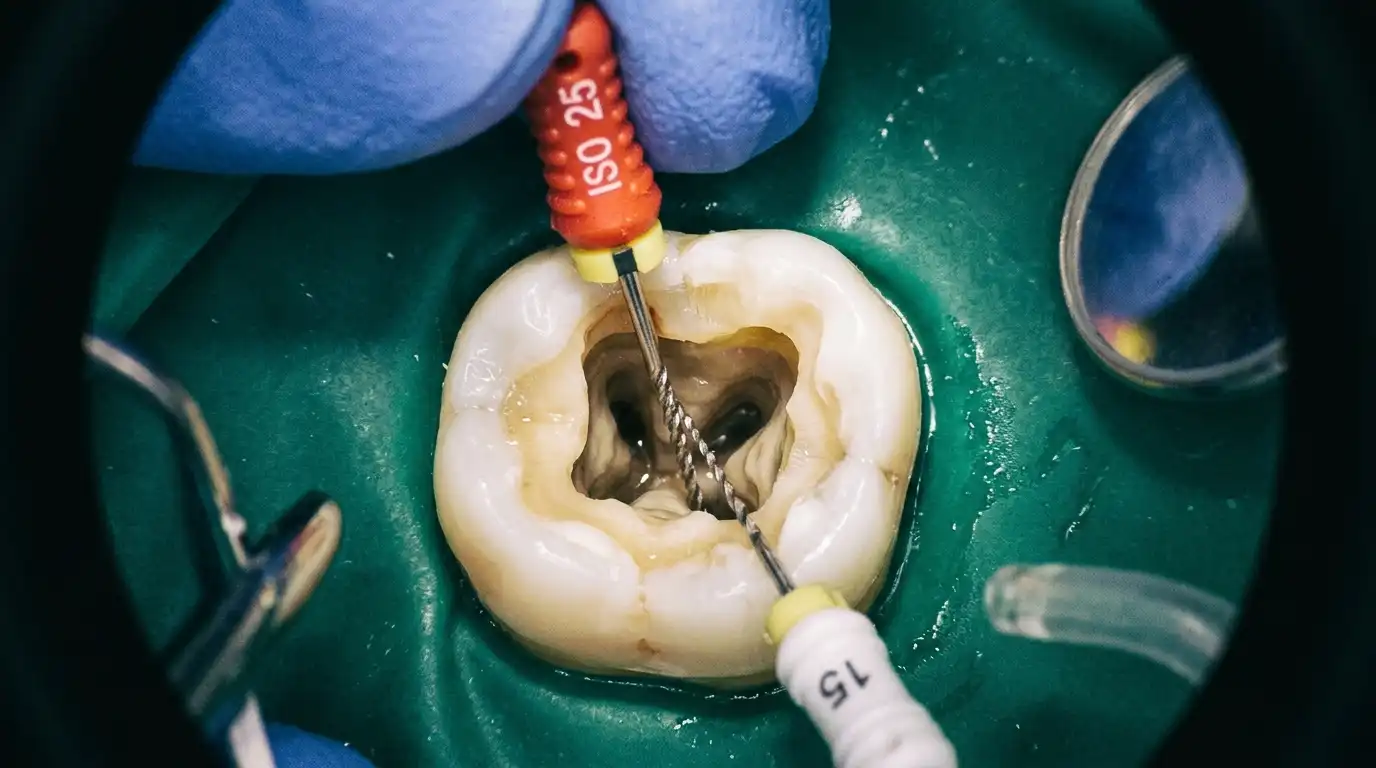
Phase 3: Microscopic Cleaning and Shaping The endodontist creates a very small access hole in the top of the tooth. Utilizing specialized endodontic microscopes and highly flexible, nickel-titanium rotary files, the dead and infected pulp is meticulously removed from the central chamber and down through the tiny, branching root canals.
As the canals are shaped, we constantly flush them with powerful antibacterial irrigants (like sodium hypochlorite) to chemically dissolve remaining tissue and kill 100% of the bacteria hiding in microscopic tubules.
Phase 4: 3D Obturation (Sealing the Tooth) Once the internal canal system is perfectly hollow, clean, and dry, leaving it empty would invite new bacteria to move in. We must hermetically seal it.
We fill the complex canal pathways with a biocompatible, rubber-like material called Gutta-Percha. This material is heated and compacted into the roots, flowing into every microscopic crevice and permanently sealing the tooth from the root tip up to the crown. Finally, a temporary or permanent filling is placed in the access hole.
5. The Critical Final Step: The Dental Crown
A root canal procedure effectively “kills” the tooth—it is no longer alive, meaning it no longer receives internal hydration or nutrients. Over the following months, the remaining hard enamel shell will naturally become increasingly dry, brittle, and structurally compromised.
Because your molars withstand up to 200 pounds of pressure during heavy chewing, a brittle, root-canaled tooth is at an extremely high risk of fracturing or splitting vertically. If a tooth splits entirely down the middle, it cannot be saved and must be extracted, rendering the entire root canal procedure useless.
To prevent this tragedy, it is the absolute standard of care to place a Dental Crown over any back tooth that has received a root canal.
- Shortly after your root canal is complete, you will transition to our restorative team.
- We will prepare the tooth by reshaping the outer shell.
- We will take digital impressions and our laboratory will mill a 100% customized, ultra-strong Porcelain or solid Zirconia crown.
- This crown acts like a protective helmet, completely encasing the brittle tooth and binding it together, restoring its original strength, biting capacity, and aesthetic beauty for decades to come.
6. Post-Treatment Recovery
The recovery from a modern root canal is incredibly mild. Once the anesthesia wears off a few hours after the procedure, the severe, throbbing pain you experienced prior to the visit will be completely gone.
You may experience a dull “bruised” feeling or mild tenderness around the tooth and jaw for 2 to 4 days. This is a normal inflammatory reaction of the bone healing around the tip of the root now that the infection source has been removed. This mild discomfort is easily managed with standard over-the-counter anti-inflammatory medications (like Ibuprofen).
You can return to work and your normal daily activities immediately. The only restriction is to avoid aggressively chewing hard, crunchy foods (like nuts or ice) on that specific tooth until your permanent protective crown has been placed.